15th Jun 2022
Latest Finding in Low T3 Syndrome from the Field of…Neuroscience?
Yes. You read that correct. There have been some amazing advances in the field of neuroscience, published March 12th, and it affects us, thyroid patients. How?Researchers in Neurosurgery were aware that patients, who were critically sick or recovering from surgery, did not do as well as others if they had low levels of the thyroid hormones T3. Surgery is the most common treatment for brain tumors, and for the sake of their surgical patients, the neuroscientists were compelled to determine how the levels of T3 effected the recovery process. Specifically, the researchers investigated if Low T3 Syndrome was associated with 1) “unfavorable medical conditions” and 2) patient anxiety/depression before and after surgery (since anxiety/depression were also associated to poor patient outcomes.) “Low T3 Syndrome is a term used to describe the finding of low blood serum concentrations of T3, which can be accompanied by abnormal T4 (thyroxine) to T3 conversion and high concentrations of reverse T3 (rT3) without any obvious sign of thyroid disease.”What did they find?
- Patients with Low T3 Syndrome were 4x as likely to display symptoms of depression before surgery.
- Low T3 Syndrome was clearly linked to poor clinical outcomes in patients who underwent brain surgery.
The primary researcher was quoted saying,”Thyroid hormone concentrations can easily be investigated in routine clinical settings. The tests are inexpensive and readily available worldwide. Thyroid hormone concentrations can be potentially relevant for risk stratification in patients undergoing surgery for brain tumors.” Read article here.
What does this mean for thyroid patients?
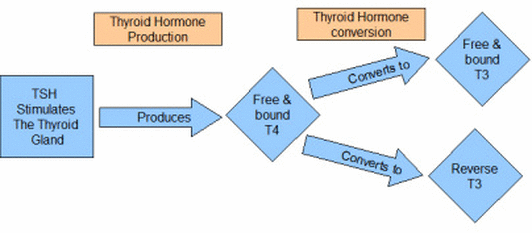
Continued research is supporting the importance of T3 in the primary functions of our body and on our mood. This article describes research that forms a clear conclusion: A patient will not thrive with a deficiency in the levels of T3 hormone or Low T3 Syndrome. Do not forget the definition of it which states, in part, that Low T3 Syndrome has “no obvious sign of thyroid disease.” Therefore, hormonal testing is necessary. This research will probably change the practice of neurosurgery and serve as support for testing the Free T3 and Reverse T3 of all patients, who are pre-operative for a brain tumors, for Low T3 Syndrome.Thyroid patients, who are diagnosed, treated, and not showing any obvious signs of thyroid disease, are often dismissed when they discuss depression or anxiety with their physicians. Thyroid patients are often referred to psychiatrists for anti-depressants and anti-anxiety medications (this study offered evidence that low levels of T3 = 4x the likelihood of depression/anxiety). Why are these doctors not instead ordering an inexpensive extended panel that includes Free T3 and Reverse T3? When I asked for these tests in addition to TSH and Free T4, my doctor recommended that I go to a “University” for such trendy treatment. The field of neurosurgery understands that the body can malfunction when there is a need to convert hormones or, as the diagram above shows, when competing hormones are made that block proper absorption/functioning of needed thyroid hormone. Currently, the American Association of Clinical Endocrinologists and American Thyroid Association jointly state that it is not necessary to test T3 and they leave it to physician’s discretion to test (read their 2012 guidelines). In today’s lawsuit crazy culture, this is like telling a physician that if they step out of your guidelines they are stepping out of “current acceptable practice” which is scary legal ground. This study is evidence that the guidelines for the treatment of hypothyroidism should make this addition to the current standard TSH and T4 lab tests:Free T3, Free T4, and Reverse T3 levels of all patients should be tested as part of a routine panel to ensure that thyroid patients do not suffer anxiety and depression. Furthermore, depression and anxiety patients should always be screened for a thyroid condition using a complete panel.
As the researchers stated, “The tests are inexpensive and readily available worldwide.”
What do YOU think? Did you ever think that you would be hoping for the field of endocrinology to catch up to the field of neuroscience in the testing of thyroid disorders?
About the Contributor
Michelle Santonastaso is a Hashimoto’s patient and was one of the co-founders of ThyroidChange. As an instructor in the field of communication and as a mother, Michelle believes continuing education is the key to improving care for all thyroid patients. With her background in speech, interpersonal communication, and healthcare administration, Michelle harnesses her training with an aim to strengthen the voice of ThyroidChange and to maximize its reach.
SIMILAR ARTICLES
More like this...

15th Jun 2022
Your Top Thyroid Questions Answered: Q&A with Dr. Lisa Hunt of Holtorf Medical Group
I had the pleasure of speaking with Lisa Hunt, D.O., an integrative physician at Holtorf Medical Group (www.holtorfmed.com) in El Segundo, CA a short while ago. I polled my audience and your top thyroid-related questions are answered here by Dr. Hunt. Dr. Hunt is a board-certified integrative physician and has extensive experience in thyroid health, hormone replacement, immune dysfunction and chronic conditions.
Read Article
15th Jun 2022
Diagnosed With a Thyroid Condition? 10 Steps to Get You Started
Pursuing proper treatment and an overall healthy lifestyle that includes eating well and exercising can help you manage a thyroid condition. But what else can you do to live well with and thrive with your condition? The information can be overwhelming and Annabel Bateman, thyroid health advocate and author, has created this guide to walk you through essential lifestyle tips once you have been diagnosed.
Read Article
15th Jun 2022
11 Tips On How To Take Your Thyroid Medication Properly
Are you taking your thyroid hormone replacement medication correctly? Did you know that how and when you take your thyroid medication can affect your ability to absorb the necessary hormone properly? In the article below, I investigate the factors that contribute to correctly (or incorrectly) taking thyroid replacement hormone and on how thyroid patients can get the most out of their medication.
Read Article